SPEND MORE TIME PREPARING FOR AN AUDIT AND LESS TIME IDENTIFYING RISK
The Compliance Risk Analyzer
The Compliance Risk Analyzer (CRA) evaluates 100% of your organization’s claims to determine the providers at risk of audit. With a few clicks, your team can see which codes may be selected for an audit and where coding practices may need improvement.
Drill Down Into the Data
The Five Main Categories Presented Are:
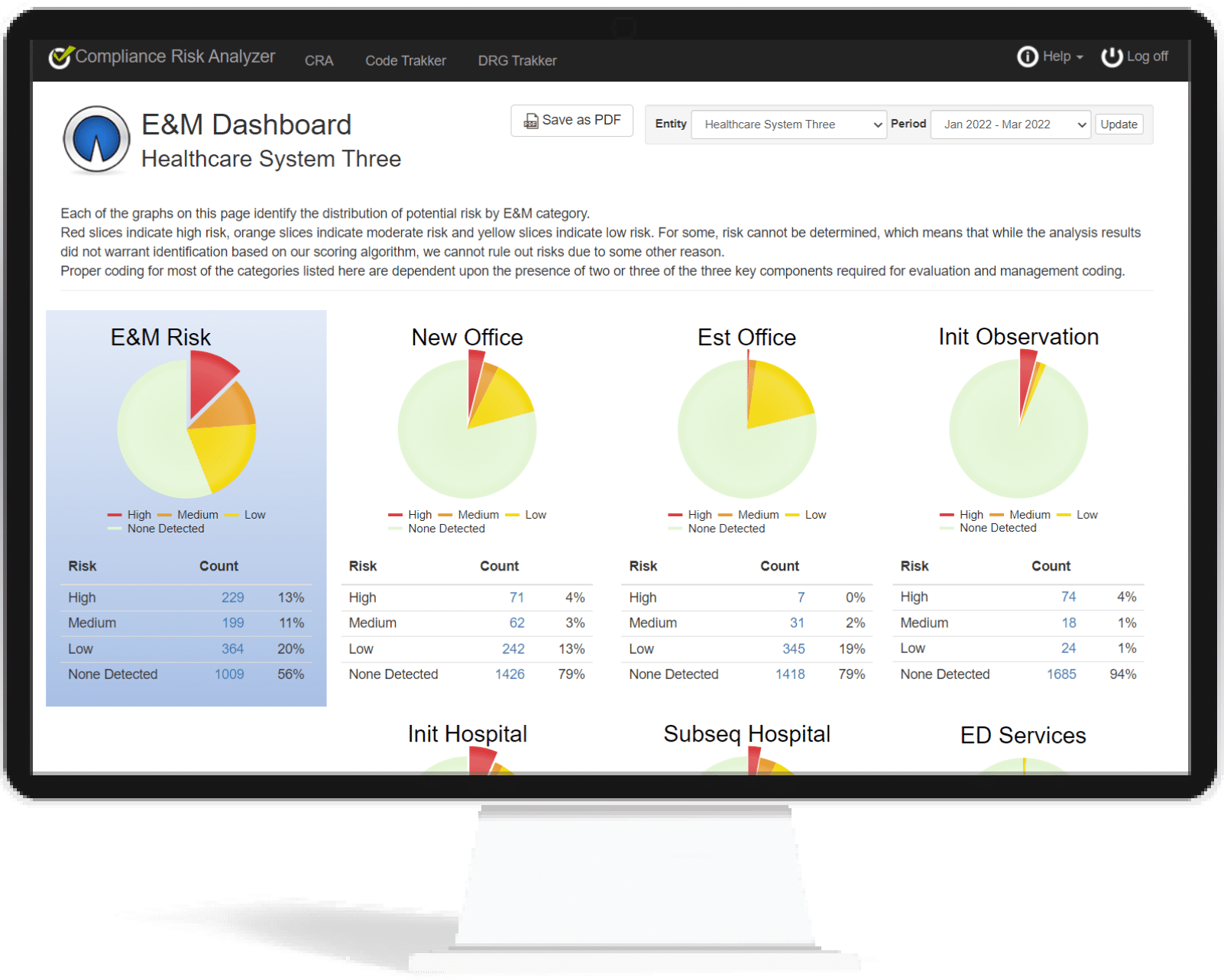
Evaluation & Management Codes
E&M Codes account for under 2% of all CPT codes. At the same time, they make up 27% of services and 40% of the total amount of payments made to providers! No wonder they are such a high-value target for both government and private payer audits. The truth is, E&M codes are the low-hanging fruit of the audit environment and as such, are pursued by the entire alphabet soup of audit entities.
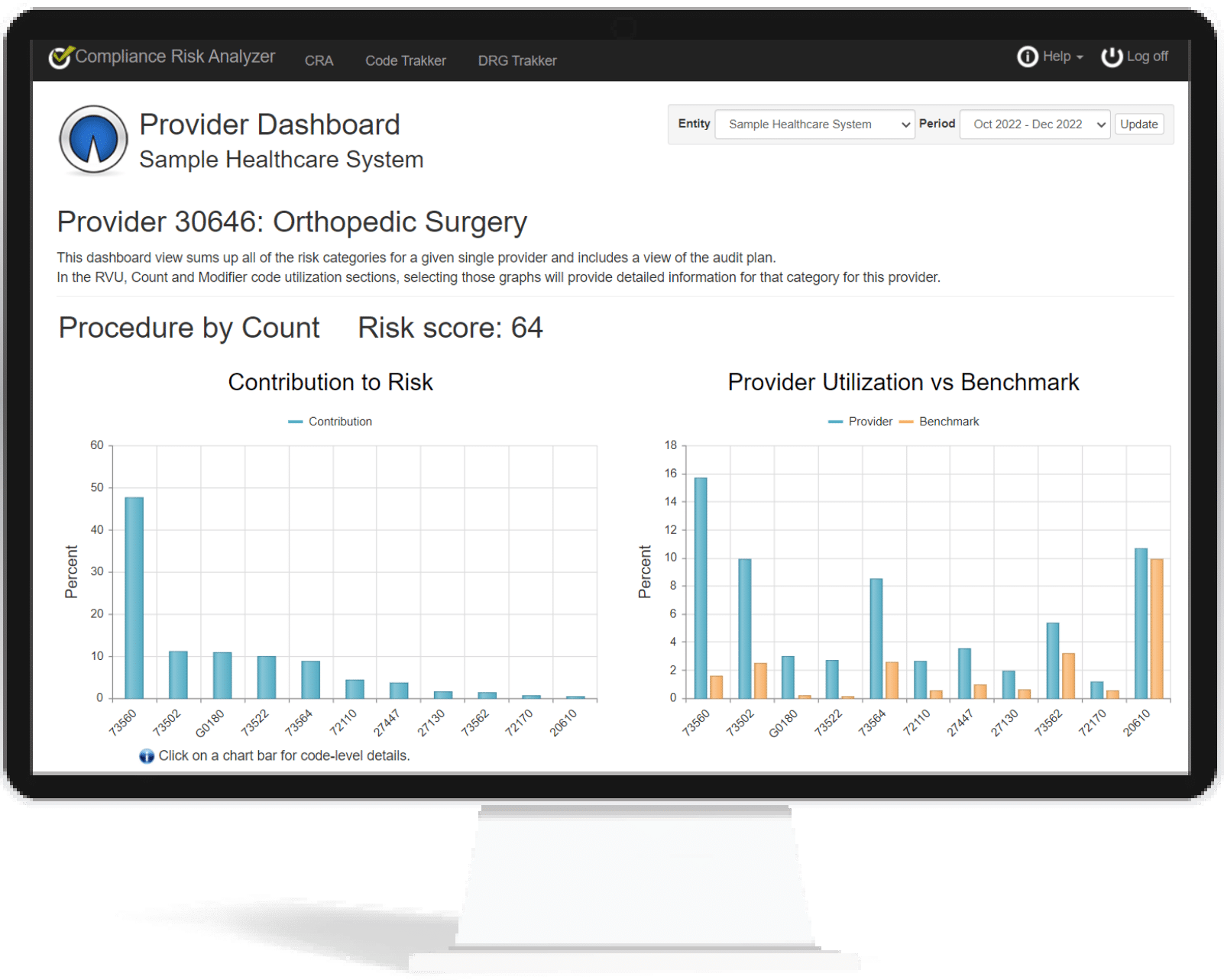
Non-E&M Procedure Codes
Unlike E&M codes, which are mutually exclusive within their own category, volume has a significant impact on risk-adjusting non-E&M codes. Regardless of predictive models, if you do something a lot more than anyone else, you are going to draw attention to yourself. And when it comes to audit risk, nobody wants to be a squeaky wheel.
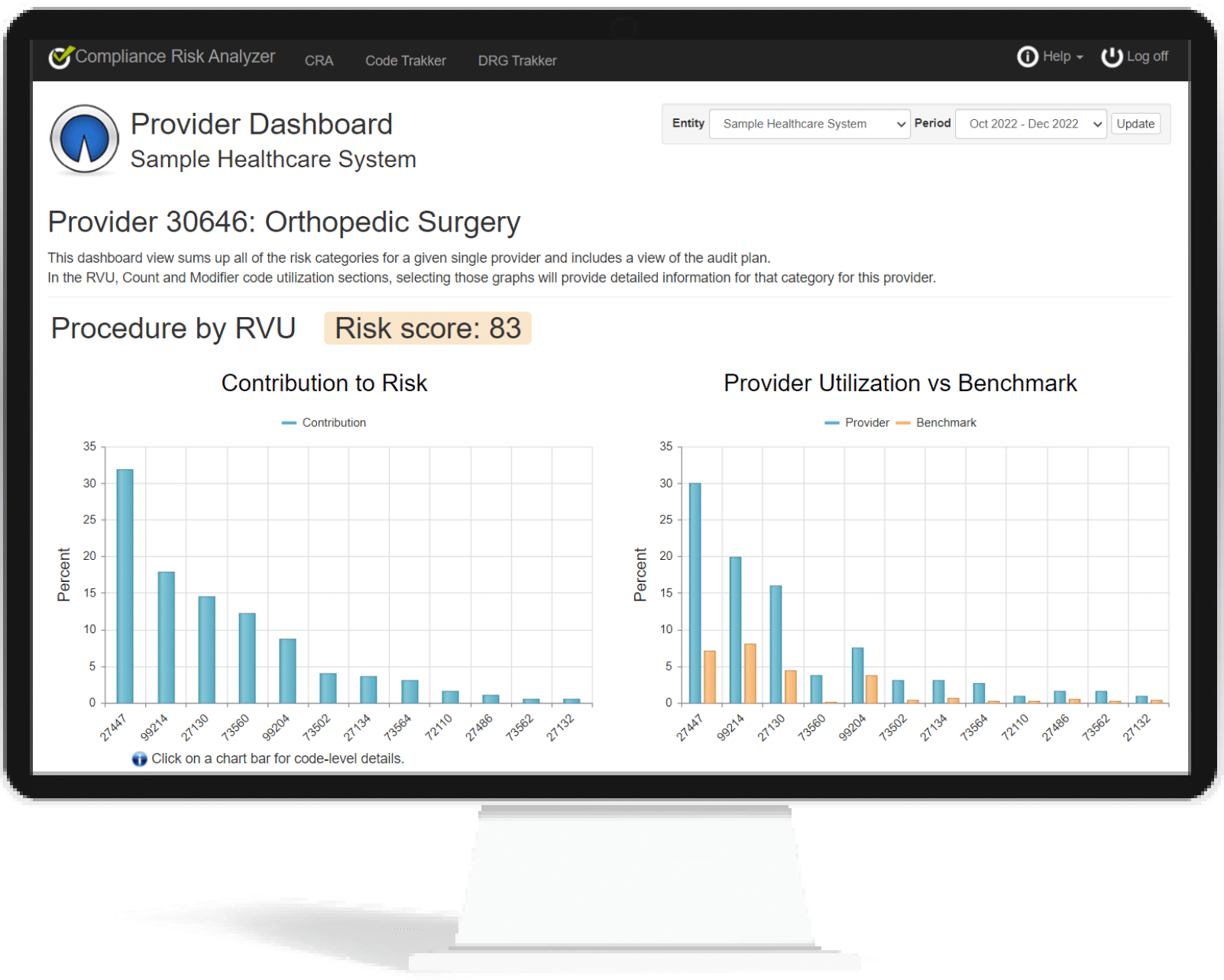
Relative Value Units (RVU)
In the private payer sector, RVUs are most often associated to costs, and costs are of major concern to private payers. That’s why many of the audits on RVU utilization are predicated by the Special Investigation Units (SIU). Unlike the government, which are subject to certain limitations regarding what they can and can’t do, private payers have a no holds barred approach to audits.
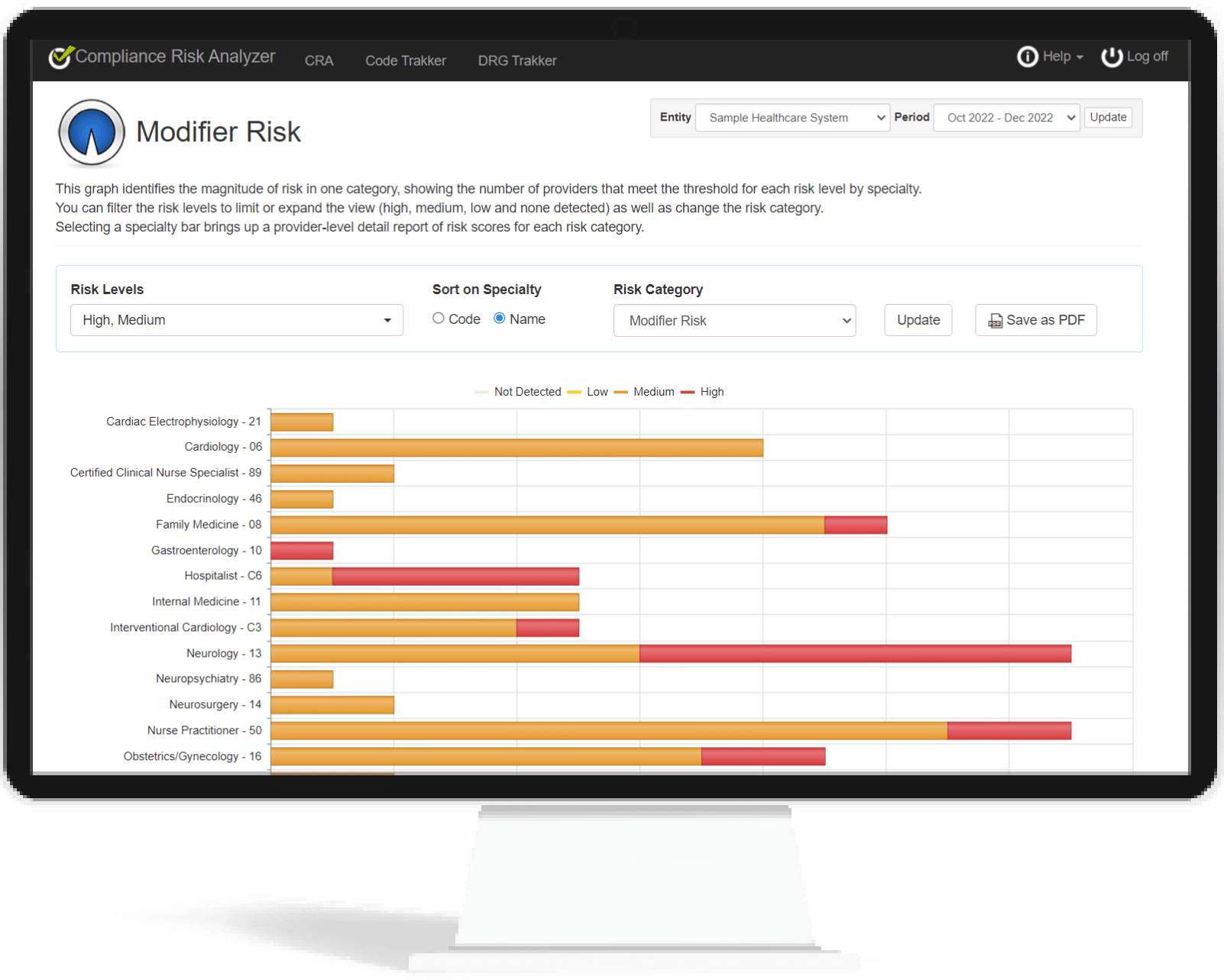
Modifiers and Modifier/Code Relationships
The use of modifiers has always been in the audit spotlight. In fact, the OIG committed the time and resources to write reports on how modifiers 25 and 59 have been abused. Over a decade later, not much has changed except the addition of many more modifiers to the potential abuse list. And when you look at how modifiers are paired to procedure codes, what you end up with is a complex web of confusion that all but requires the use of an expert system to untangle.
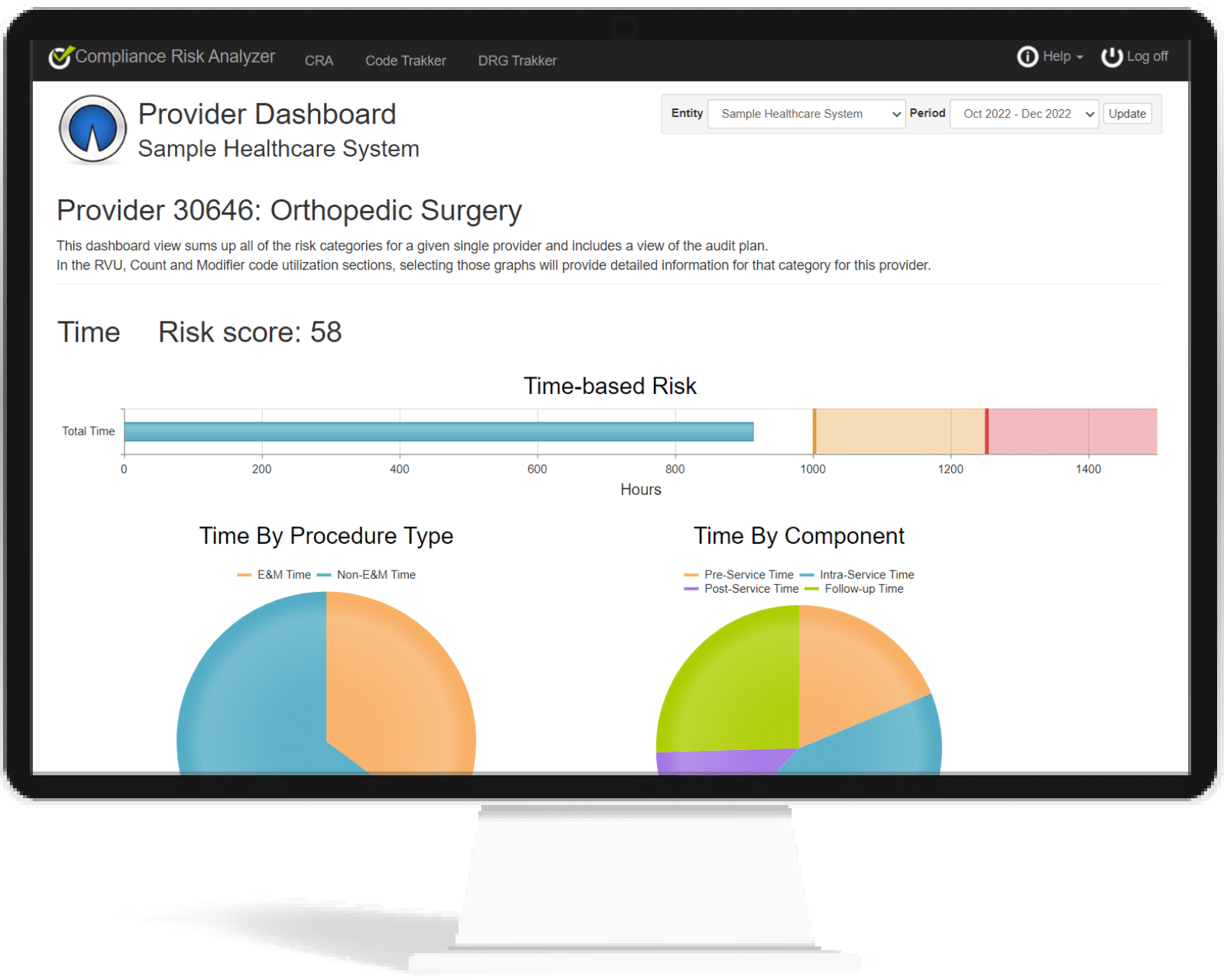
Providers' Assessed Work-Time
Provider assessed work-time is primarily the purview of the Office of Inspector General (OIG) and Department of Justice (DOJ). Most audits that are predicated on time are based on a referral from another audit entity, like a RAC or a UPIC. And while one can argue as to the accuracy of the time database, the government doesn’t care. It gives them probable cause to investigate the provider and these types of audits always leave a mark.
CRA also provides you with a composite score under Visible Risk to give you an idea of the organization’s overall health. As you identify which areas you’d like to look further into, clicking the dashboard takes you deeper into which categories, specialties, and even providers are at the highest risk for an audit.
- At a glance, your team can see what areas present the most risk.
- Prioritizes the procedure and modifier codes for each provider at risk.
- Identifies potentially under-coded E&M services that may represent a revenue opportunity for the practice.
- Monitor the results of your remediation and education efforts.
In a Matter of Seconds
You Can Identify Thousands Of Potential Risks Without Opening A Single Chart.
Book a DemoCross Referenced Cohort Data
Every provider has a peer group associated with them—a group of similar providers that the FPS system uses to compare coding habits. CRA takes this a step further by including data from an independent cohort group, thus creating the perfect “average” provider for every specialty. By comparing your data against thousands of similar providers, the CRA classifies claims into one of three risk levels: low, medium, or high. This presents you with a clear idea of how the FPS will view your providers’ coding habits compared to their peers’ habits.